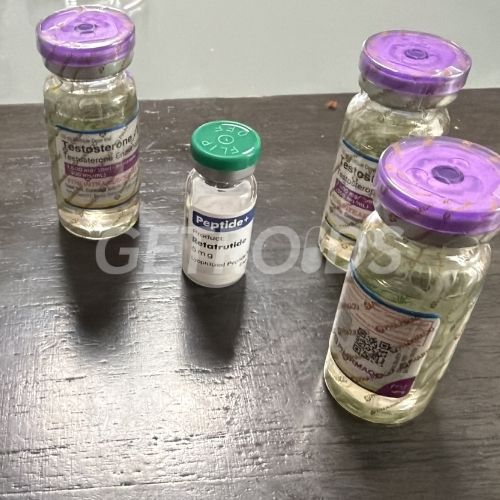
What is TESTOSTERONE UNDECANOATE?
Pharmacological action
Androgen. Testosterone undecanoate is an ester of the endogenous androgen, testosterone. The active form, testosterone, is formed by cleavage of the side chain.
Testosterone is a male sex hormone that has the entire spectrum of bioactivity necessary for the formation and maintenance of androgenic functions. It is synthesized mainly in the testicles and, to a lesser extent, in the adrenal cortex. Testosterone ensures the formation of male characteristics during fetal development and early childhood; during puberty - the development of male genital organs and secondary sexual characteristics. Further testosterone ensures the maintenance of the male phenotype and androgen-dependent functions (e.g., spermatogenesis, reproductive glands).
Insufficient secretion of testosterone leads to male hypogenitalism, which is characterized by low concentration of testosterone in a blood serum. Some symptoms associated with male hypogenitalism include, but are not limited to, erectile dysfunction, decreased sex drive, fatigue, depressed mood, absence, underdevelopment or regression of secondary sexual characteristics, and an increased risk of osteoporosis. Exogenous androgens are prescribed to increase insufficient levels of endogenous testosterone and reduce symptoms of hypogenitalism.
Depending on the target organ, the nature of testosterone's action is mainly androgenic (for example, prostate gland, seminal vesicles, epididymis) or protein-anabolic (muscles, bones, hematopoietic system, kidneys, liver).
The effects of testosterone in some organs occur after the peripheral conversion of testosterone to estradiol, which then binds to estrogen receptors in the nuclei of target cells (for example, pituitary gland, fat tissue, brain, bone and testicular Leydig cells).
In the bodies of men suffering from hypogenitalism, the use of androgens reduces body fat mass, increases lean body mass, and also prevents bone tissue loss. Androgens can improve sexual function and also have a positive psychotropic effect, improving mood.

Pharmacokinetics
Testosterone decanoate is introduced into body as an intramuscular (i.m.) depot injection. Therefore, there is no first pass effect. After an intramuscular injection of an oil solution of testosterone undecanoate, it is gradually released from the depot and is almost completely split by serum esterases into testosterone and undecanoic acid. An increase in serum testosterone concentrations relative to baseline values can be detected as early as the next day after injection. After the first i.m. injection of 1000 mg testosterone undecanoate given to men with hypogenitalism, an average value of maximum concentration in blood (Cmax) of 38 nmol/L (11 ng/ml) was observed after 7 days. The concentration in blood had been gradually increasing with subsequent injections. The average maximum and average minimum testosterone concentrations at steady state were approximately 37 nmol/L (11 ng/mL) and 16 nmol/L (5 ng/mL), respectively.
About 98% of circulating testosterone is bound in serum to sex hormone-binding globulin (SHBG) and albumin. Only the free fraction of testosterone is considered biologically active. Testosterone, formed from testosterone undecanoate as a result of cleavage of the ester bond, is metabolized and excreted from the body in the same ways as endogenous testosterone. Undecanoic acid is metabolized by beta-oxidation in the same way as other aliphatic carboxylic acids. The main active metabolites of testosterone are estradiol and dihydrotestosterone.
Testosterone undergoes significant metabolism in and outside the liver. After injection of labeled testosterone, about 90% of the radioactivity is determined in the urine in the form of glucuronide and sulfate acid conjugates, and 6% after passage of the enterohepatic circulation is found in the feces. Products detected in urine include androsterone and etiocholanolone. After i.m. injection, the depot T1/2 is 90±40 days.
Indications of the active substance TESTOSTERONE UNDECANOATE
Replacement therapy for hypogenitalism in men, in cases where testosterone deficiency is confirmed by clinical symptoms and the results of biochemical studies.
Dosage schedule
Injected intramuscularly as a depot injection at a dose of 1 g once every 10-14 weeks.
Before starting treatment, the level of testosterone in plasma should be determined. The first interval between injections can be shortened, but should be at least 6 weeks. Steady state concentration (ssc) at this dose is achieved quickly.
Side effects
Most common: acne, pain at the injection site.
Blood and lymphatic system: often - polycythemia; infrequently - increased hematocrit, increased number of red blood cells, increased hemoglobin levels.
Immune system: rarely - hypersensitivity.
Metabolism: often - weight gain; uncommon - increased appetite, increased levels of glycosylated hemoglobin, hypercholesterolemia, increased levels of triglycerides in the blood, increased levels of cholesterol in the blood.
Mental side: infrequently - depression, emotional disturbances, insomnia, anxiety, aggressiveness, irritability.
Nervous system: infrequently - headache, migraine, tremor.
Respiratory system: infrequently - bronchitis, sinusitis, cough, shortness of breath, snoring, dysphonia.
Cardiovascular system: often - hot flashes; infrequently - dysfunction of the cardiovascular system, arterial hypertension, dizziness.
Digestive system: infrequently - diarrhea, nausea, abnormal liver function tests, incl. increased aspartate transaminase (AST) activity.
Skin and subcutaneous tissues: often - acne; uncommon - alopecia, erythema, rash, papular rash, itching, dry skin.
Musculoskeletal system: infrequently - arthralgia, pain in the limbs, muscle spasms, muscle tension, myalgia, musculoskeletal rigidity, increased creatine kinase (CK) activity in the blood.
Urinary system: uncommon - decreased volume of urine excreted, urinary retention, dysfunction of the urinary tract, nycturia, dysuria.
Reproductive system: often - increased prostatic specific antigen (PSA) levels, pathological results of examination of the prostate gland, benign prostatic hyperplasia; uncommon - prostate intraepithelial neoplasia, prostate induration, prostatitis, prostate dysfunction, increased libido, decreased libido, testicular pain, breast pain, breast induration, gynecomastia, increased estradiol levels, increased free testosterone levels in the blood, increased testosterone levels in the blood.
General reactions: uncommon - increased fatigue, asthenia, hyperhidrosis, night sweats.
Contraindications
Hypersensitivity to testosterone undecanoate, androgen-dependent prostate or breast carcinoma, current or history of liver tumors; hypercalcemia accompanying malignant tumors. Contraindicated for use in women, children and adolescents under 18 years of age.
Patients with apnea syndrome, arterial hypertension, severe liver, kidney and heart failure, coronary artery disease, prone to edema, thrombophilia, epilepsy, migraine.
Use during pregnancy and breastfeeding: Not intended for use in women.
Use for liver dysfunction: Use with caution in patients with liver failure.
Use for renal impairment: Use with caution in patients with renal failure.
Use in children: Contraindicated for use in children and teenagers under 18 years of age.
Use in elderly patients: The limited available data do not indicate the need for dose adjustment in elderly patients.
Special instructions:
Testosterone undecanoate should only be used if hypogenitalism (hyper- and hypogonadotropic) has been verified, and if other etiologies that could cause the development of symptoms have been excluded before starting treatment.
Testosterone deficiency must be confirmed by the presence of clinical signs (including regression of secondary sexual characteristics, changes in body composition, asthenia, decreased libido, erectile dysfunction) and the results of two separate measurements of testosterone concentration in the blood.
Currently, there is no generally accepted opinion on testosterone reference values for patients of different ages. However, it should be taken into account that physiologically the concentration of testosterone in the blood serum becomes lower with age.
Before starting treatment with drugs containing testosterone, a thorough examination should be carried out to exclude the presence of prostate cancer. Regular and careful monitoring of the condition of the mammary glands and prostate gland is recommended (conducting a digital rectal examination of the prostate and determining the prostatic specific antigen (PSA) concentration at least once a year, and in elderly patients and patients with risk factors for prostate cancer (including a family history of anamnesis) - at least 2 times a year.
Testosterone concentrations should be monitored at the beginning of treatment and throughout the entire period of therapy at regular intervals. Individual dose adjustment is required to ensure that the required testosterone concentration is maintained.
In patients on long-term androgen therapy, regular determination of hematocrit and hemoglobin content, as well as liver enzyme activity and lipid profile, is recommended. When using androgens, it is recommended to measure testosterone concentrations in the same laboratory.
When using androgens, the risk of developing benign prostatic hyperplasia may increase, as well as accelerated progression of existing hyperplasia and subclinical prostate cancer.
Use with caution in cancer patients at risk of hypercalcemia (and associated hypercalciuria) due to bone metastases. Regular monitoring of serum calcium concentrations is recommended in these patients.
During the use of sex hormones, which include testosterone, benign and malignant liver tumors were recorded.
If testosterone undecanoate causes severe pain in the upper abdomen, liver enlargement, or signs of intra-abdominal bleeding, the differential diagnosis should take into account the possibility of a liver tumor.
As a general rule, the risk of bleeding should always be considered when administering testosterone undecanoate IM to patients with acquired or hereditary bleeding disorders.
Testosterone should be used with caution in patients with thrombophilia or other risk factors for venous thromboembolism (VTE), since post-marketing studies have reported cases of thrombosis (eg, deep vein thrombosis, pulmonary embolism, ocular thrombosis) with the use of testosterone preparations in such patients. Cases of VTE have been reported in patients with thrombophilia even during anticoagulant therapy, and therefore the need to continue testosterone use after the first episode of thrombosis should be strictly assessed. If treatment is continued, additional measures must be taken to minimize the individual risk of VTE.
In patients with severe cardiac, hepatic or renal impairment or coronary artery disease, testosterone use may cause serious complications characterized by edema with or without congestive heart failure. In this case, therapy should be stopped immediately.
Caution is required in patients prone to the development of edema, for example in cases of severe cardiac, hepatic and renal failure or coronary artery disease. Testosterone use may cause sodium and fluid retention in the body. If severe complications develop, characterized by edema with or without congestive heart failure, therapy should be discontinued immediately.
Increased insulin sensitivity may occur in patients taking androgens who achieve normal plasma testosterone concentrations after replacement therapy.
Some clinical signs: irritability, nervousness, weight gain, prolonged or frequent erections may indicate excessive androgen exposure, requiring dose adjustment.
Athletes receiving testosterone replacement therapy for primary and secondary male hypogenitalism should be informed that testosterone undecanoate medicinal product contains an active substance that may cause a positive reaction in anti-doping tests.
Androgens are not used to enhance muscle development in healthy subjects, nor to enhance physical performance.
Cases of abuse of testosterone preparations have been reported, usually in doses exceeding those recommended for approved indications and in combination with other anabolic androgenic steroids. Abuse of testosterone drugs can cause dependence, as well as withdrawal syndrome if the dose is significantly reduced or abruptly discontinued. Abuse of testosterone preparations, along with other anabolic androgenic steroids, can lead to serious adverse reactions from the cardiovascular system (in some cases fatal), liver and/or mental disorders. Abuse of testosterone drugs and other anabolic androgenic steroids poses significant health risks and is highly discouraged.
Drug interactions
Interaction with drugs that induce microsomal enzymes (for example, barbiturates) is possible, which can lead to an increase in testosterone clearance.
Increases in serum concentrations of oxyphenbutazone have been reported.
Testosterone and its derivatives may enhance the pharmacological effect of indirect oral anticoagulants, coumarin derivatives, which may lead to the need for dose adjustment.
Careful monitoring of patients receiving indirect oral anticoagulant therapy with regular determination of prothrombin time and international normalised ratio (INR) is necessary, especially at the beginning and end of testosterone therapy.
Androgens can enhance the hypoglycemic effect of insulin. It may be necessary to reduce the dose of the hypoglycemic drug.
When using testosterone simultaneously with adrenocorticotrophic hormone (ACTH) or glucocorticosteroids (GCS), the risk of developing edema increases. Therefore, these combinations should be used with caution, especially in patients with heart or liver disease or if the patient is predisposed to developing edema.
Sources:
https://planetazdorovo.ru/
https://sportwiki.to/
Customer Reviews
Discover real user experiences and explore our products.